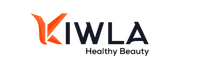What Are Biofilms and Why Are They So Hard to Get Rid Of?
Biofilms are fascinating yet challenging structures that have significant implications for health, industry, and the environment. They are communities of microorganisms that adhere to surfaces and are embedded in a protective matrix. Understanding what biofilms are and why they are so difficult to eliminate can help us address the various problems they pose, from chronic infections to industrial fouling.
What Are Biofilms?
Biofilms are complex aggregates of bacteria, fungi, and other microorganisms that stick to surfaces in natural, industrial, and clinical settings. These microorganisms produce a slimy, protective layer made primarily of polysaccharides, proteins, and nucleic acids. This matrix not only anchors the microbes to the surface but also serves as a shield against environmental stressors, including antibiotics and the immune system.
Formation of Biofilms:
The process of biofilm formation generally occurs in several stages:
- Initial Attachment: Microorganisms adhere to a surface using appendages like pili or fimbriae.
- Colonization: Once attached, these microorganisms multiply and begin to produce the extracellular matrix.
- Mature Biofilm Development: As the biofilm grows, it develops a complex structure with channels that allow nutrients and waste products to flow through.
- Dispersal: Parts of the biofilm can detach and spread to new surfaces, allowing the biofilm to expand and colonize new areas.
What Makes Biofilms So Challenging to Remove?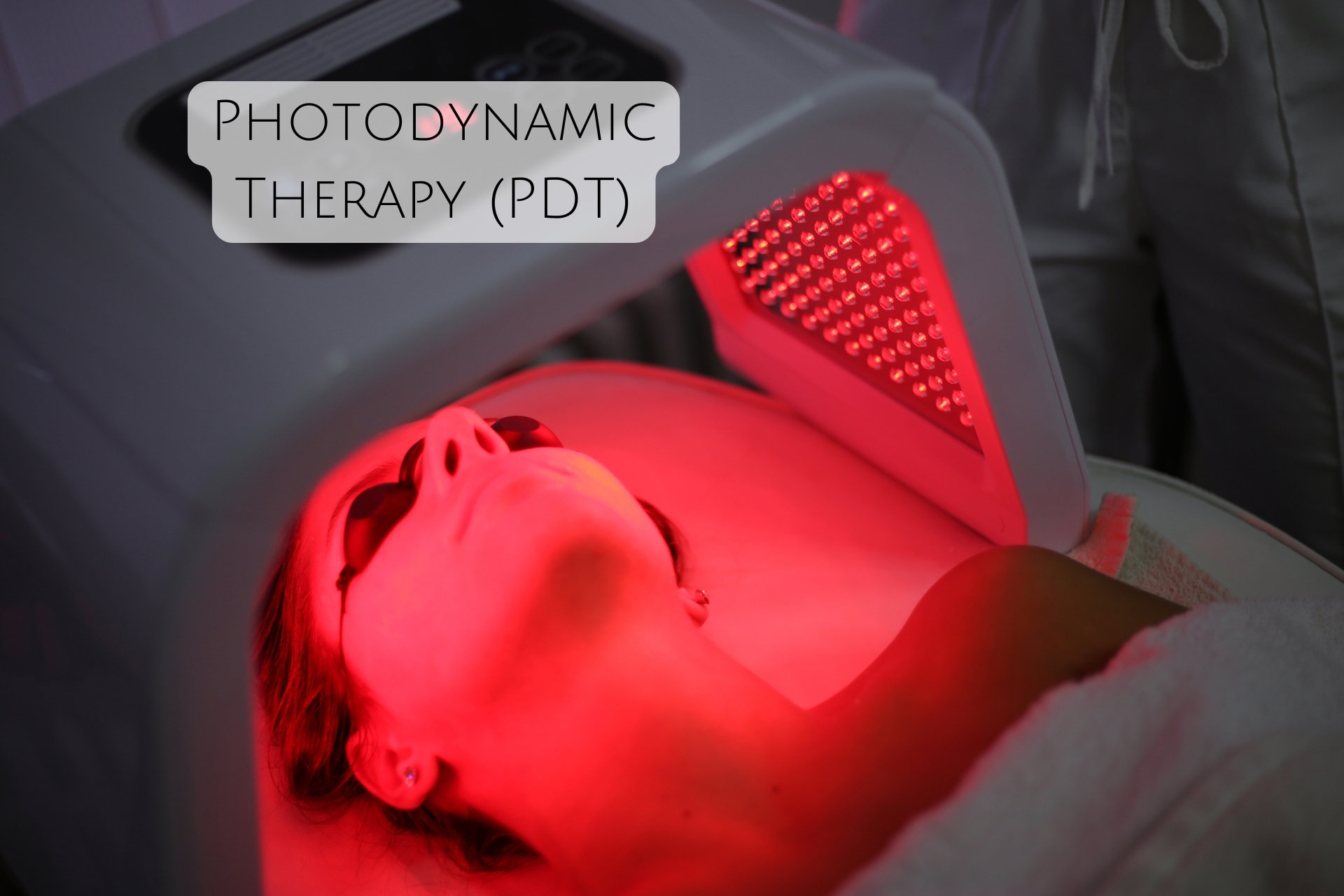
Biofilms pose unique challenges in both medical and industrial contexts, primarily due to their protective properties and adaptive characteristics. Here are several reasons why they are particularly challenging to eliminate:
1. Protection from Antimicrobials:
The extracellular matrix acts as a physical barrier, making it difficult for antibiotics and disinfectants to penetrate and effectively kill the microorganisms within. This protection allows bacteria within biofilms to survive even in the presence of high concentrations of antimicrobial agents.
2. Altered Microbial Metabolism:
Microorganisms in biofilms often exhibit altered metabolic states, making them less susceptible to antibiotics that target actively growing cells. Some bacteria can enter a dormant state within biofilms, further reducing the effectiveness of treatments.
3. Genetic Exchange:
Biofilms can facilitate horizontal gene transfer among bacteria, allowing them to share resistance genes.
4. Environmental Resilience:
Biofilms can withstand extreme environmental conditions, including changes in temperature, pH, and nutrient availability. Their ability to adapt to various stresses makes them resilient and hard to eliminate.
5. Chronic Infections:
In a medical context, biofilms are associated with chronic infections, such as those found in cystic fibrosis patients or in implanted medical devices like catheters and prosthetic joints. The protective nature of biofilms allows them to persist despite treatment, leading to recurring infections and complications.
Strategies for Managing Biofilms:
Given the challenges posed by biofilms, effective management strategies are essential. Here are some approaches currently being explored:
1. Mechanical Disruption:
Physically removing biofilms through scraping or high-pressure washing can help reduce their presence, particularly in industrial settings.
2. Use of Biocides:
While traditional antibiotics may be ineffective, novel biocides and antimicrobial agents that target biofilm structures are being developed. These agents can penetrate the matrix or disrupt biofilm formation.
3. Enzymatic Treatments:
Certain enzymes can break down the extracellular matrix, making it easier for antimicrobials to reach the microorganisms. Research is ongoing to identify effective enzymes for biofilm control.
4. Combination Therapy:
Using a combination of antibiotics and other agents can enhance treatment efficacy. For instance, pairing antibiotics with biofilm-disrupting agents may yield better results than either treatment alone.
5. Preventive Measures:
Preventing biofilm formation is crucial in both healthcare and industrial settings. Regular cleaning, sterilization, and the use of materials that resist biofilm formation can help mitigate the issue.
Conclusion:
Biofilms are complex microbial communities that pose significant challenges across various fields. Their ability to protect microorganisms from antimicrobial agents and facilitate the spread of resistance makes them difficult to eliminate. However, through a combination of mechanical, chemical, and preventive strategies, we can better manage biofilms and reduce their impact on health and industry. Understanding these structures is essential for developing effective treatments and maintaining clean, safe environments.
Recent Posts
-
Scalp Therapy Isn’t Just a Trend—It’s the Next Big Haircare Routine
Introduction:Scalp therapy isn't just a trend—it's the next big haircare routine that's changing how
-
Seed-Cycling, Cold Plunges & Breathwork: Why Indians Are Embracing These ‘Biohacks’
Introduction: India has always had a rich tradition of holistic wellness — from Ayurveda and pranay
-
Sustainable Beauty: How to Build an Eco-Friendly Vanity in India
Introduction: In a world increasingly driven by the urgent need for sustainability, even our beauty