The Mind-Body Connection: How Blood Sugar Affects Your Mood and Metabolism
Introduction:
In today's fast-paced world filled with refined foods, chronic stress, and sedentary habits, blood sugar has become epidemic. The consequences ripple through every aspect of health—from stubborn weight gain and energy crashes to mood swings, anxiety, and depression. Blood sugar balance sits at the foundation of metabolic health, influencing far more than just glucose levels. It controls appetite, energy production, brain chemistry, hormonal balance, and even emotional resilience.
Your blood sugar naturally rises and falls throughout the day as you eat, move, or rest. But modern lifestyles—high-carbohydrate meals, sugary snacks, stress, irregular sleep, and long work hours—create extreme spikes and crashes. These disruptions don’t just affect your weight; they affect how you feel, think, and function daily. Understanding why stable glucose matters—and learning how to achieve it—is one of the most powerful interventions for reclaiming vitality, mental clarity, and lasting weight management.
What Blood Sugar Actually Is — and How It Affects Your Body: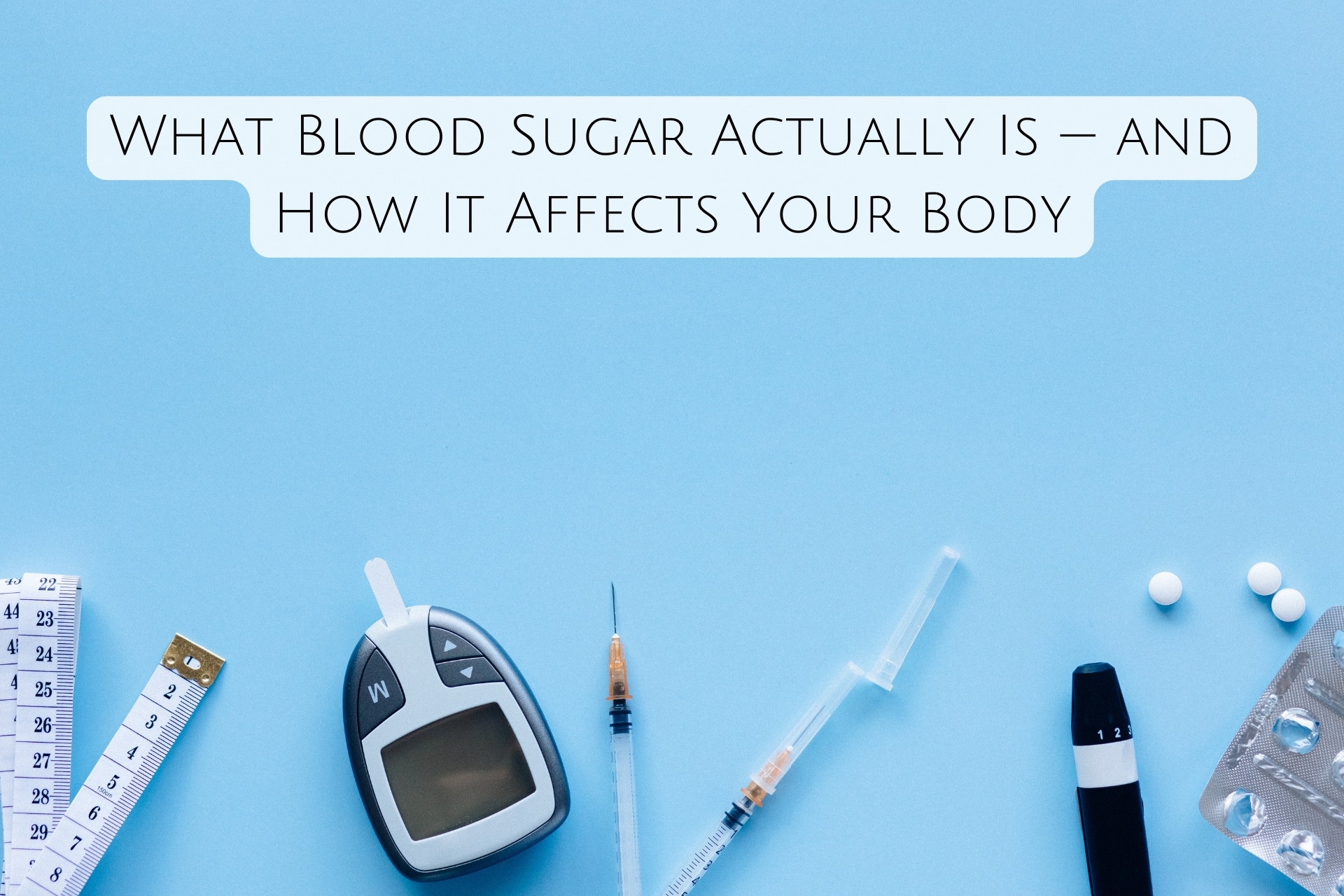
Blood sugar, or blood glucose, is the concentration of glucose—a simple sugar derived from carbohydrate digestion—circulating in your bloodstream. When you eat carbohydrates (bread, fruit, sugar), your digestive system breaks them down into glucose molecules, which are absorbed into the bloodstream. The pancreas responds by secreting insulin, a hormone that acts as a "key," allowing glucose to enter muscle, fat, and liver cells where it's used for immediate energy or stored for later use. This tightly regulated system maintains blood glucose within a narrow range (70-100 mg/dL fasting, up to 140 mg/dL after meals) to ensure optimal cellular function.
However, the composition and timing of foods you eat dramatically influence how fast glucose enters the bloodstream. Refined carbohydrates and sugary foods cause rapid spikes, triggering large insulin secretions. Whole foods with fiber, protein, and healthy fats result in slower, gentler glucose absorption and smaller insulin responses. When blood glucose remains chronically elevated, the pancreas works overtime, eventually becoming less responsive—a condition called insulin resistance. In this state, cells ignore insulin's signals, glucose remains in the bloodstream, and the pancreas produces even more insulin in a futile attempt to lower blood sugar.
The immediate effects of blood sugar changes are felt throughout the body. High blood glucose triggers thirst, increased urination, and inflammation. Low blood glucose triggers shakiness, sweating, hunger, and adrenaline release. Over time, chronic dysregulation damages blood vessels, nerves, and organs, increasing risk for cardiovascular disease, kidney disease, retinopathy, and neuropathy. Additionally, poor blood sugar control promotes weight gain through increased fat storage and appetite dysregulation, accelerates skin aging through AGE formation, and impairs brain function through reduced neurotransmitter production and neuroinflammation.
Why Blood Sugar Balance Is Essential for Weight Management:
Insulin is fundamentally an anabolic hormone—it signals the body to store energy as fat. When insulin levels remain chronically elevated due to poor blood sugar control, the body remains in "storage mode," making weight loss nearly impossible despite caloric restriction. Conversely, stable blood sugar and lower insulin levels shift the body toward fat burning and energy utilization rather than storage.
Blood sugar stability also directly controls appetite hormones—ghrelin (hunger) and leptin (satiety). When glucose crashes, ghrelin surges, triggering intense cravings and food-seeking behavior, particularly for high-calorie, high-sugar foods that quickly raise blood glucose. This creates a vicious cycle: blood sugar spike → insulin surge → glucose crash → intense hunger and cravings → overeating → another spike. People caught in this cycle often gain weight despite eating "less," because their hormonal signals are dysregulated.
By maintaining stable blood glucose through low-glycemic foods, regular exercise, adequate protein, and stress management, insulin levels normalize, appetite hormones balance, and the body naturally gravitates toward its ideal weight. Studies show that individuals with stable blood sugar lose weight more easily, maintain lean muscle mass, and experience fewer cravings—making sustainable weight management achievable without exhausting willpower or extreme restriction.
Symptoms of Blood Sugar Imbalance:
Blood sugar imbalances often manifest through distinct physical and emotional symptoms, serving as vital signals from the body. Common signs of hypoglycemia include shakiness, irritability, fatigue, and difficulty concentrating, while hyperglycemia may present with increased thirst, frequent urination, and blurred vision. Mood disturbances such as anxiety or depression can also arise from blood sugar fluctuations, highlighting the intricate mind-body connection. Early recognition of these symptoms allows timely intervention, enabling individuals to restore balance through dietary adjustments, exercise, and stress management. Awareness and responsiveness to these bodily cues are essential for maintaining optimal metabolic and emotional health.
How Blood Sugar Impacts Mood, Mental Health & Cognitive Performance:
The brain's dependence on glucose makes it extraordinarily vulnerable to blood sugar fluctuations. When glucose is adequate and stable, neurons efficiently produce neurotransmitters—serotonin (mood stability and happiness), dopamine (motivation and reward), GABA (relaxation and focus), and noradrenaline (alertness). High serotonin and dopamine levels support positive mood, motivation, and pleasure; adequate GABA supports calmness; and balanced noradrenaline supports sustained attention and mental clarity.
However, blood sugar crashes deplete these neurotransmitters, leaving individuals feeling depressed, anxious, irritable, unmotivated, and unable to concentrate. Conversely, chronic hyperglycemia damages neurons through oxidative stress and inflammation, impairing the neural connections essential for memory, learning, and emotional regulation. Research demonstrates that people with high glycemic variability (frequent blood sugar swings) report significantly higher rates of depression, anxiety, mood swings, and cognitive dysfunction compared to those with stable glucose.
The relationship between blood sugar and mood is so direct that some mental health professionals now screen for blood sugar dysregulation in patients with mood disorders. Studies show that improving blood glucose control through dietary modifications and exercise significantly reduces depression and anxiety symptoms and improves cognitive performance—sometimes as effectively as medications. This reveals that for many people struggling with mood and focus, the root cause isn't biochemical depression or ADHD but rather metabolic dysregulation—and the solution lies in stabilizing blood sugar.
Daily Habits That Support Blood Sugar Balance:
1. Eat Protein, Fat, and Fiber at Every Meal:
Prioritize whole foods containing protein (chicken, fish, eggs, legumes, tofu), healthy fats (avocado, nuts, olive oil), and fiber (vegetables, fruits, whole grains). These macronutrients slow glucose absorption, preventing spikes and crashes. Aim for at least 20-30g of protein and 10-15g of fiber per meal.
2. Choose Low-Glycemic Carbohydrates:
Replace refined carbs (white bread, pastries, sugary cereals) with low-glycemic options (oats, sweet potatoes, legumes, quinoa, non-starchy vegetables). Low-glycemic foods release glucose slowly, preventing the insulin surges that lead to crashes and cravings.
3. Eat in the Right Order:
Consume vegetables and protein first, then healthy fats, and carbohydrates last. This "food order" significantly reduces glucose spikes by up to 70% compared to eating in reverse order.
4. Move Your Body Regularly:
Exercise, especially after meals, dramatically improves insulin sensitivity. Even 10-15 minutes of walking after eating lowers blood glucose spikes by 20-30%. Resistance training builds muscle, which acts as a glucose sink, improving long-term blood sugar control.
5. Manage Stress and Sleep:
Chronic stress elevates cortisol, which increases blood glucose and impairs insulin sensitivity. Poor sleep has the same effect. Prioritizing 7-9 hours of quality sleep and daily stress-reduction practices (meditation, yoga, breathing) are essential for metabolic health.
6. Avoid Ultra-Processed Foods & Liquid Sugars:
Eliminate or minimize sodas, energy drinks, packaged snacks, and desserts. These foods cause rapid glucose spikes, triggering intense insulin responses and subsequent crashes. Even "healthy" packaged foods often contain hidden sugars—always check labels.
7. Add Vinegar or Lemon to Meals:
Acetic acid (in vinegar) and citric acid (in lemon) slow glucose absorption and can reduce blood sugar spikes by up to 30%. Add a tablespoon of apple cider vinegar or squeeze of lemon juice to meals.
8. Stay Hydrated:
Drinking plenty of water supports kidney function and helps regulate blood glucose. Dehydration can falsely elevate blood glucose readings and worsen insulin resistance.
9. Monitor & Personalize:
Consider using a continuous glucose monitor (CGM) temporarily to identify which foods spike your glucose. Individual responses vary—what causes a spike in one person may not in another. Personalization based on your unique glucose patterns is key.
10. Consistency Over Perfection:
Small, consistent habits compound into major metabolic improvements. Rather than pursuing extreme dietary restrictions, focus on sustainable daily practices that support stable glucose—you'll see results in energy, mood, mental clarity, and weight within 2-4 weeks.
Kiwla’s Blood Sugar Balance Essentials:
Kiwla empowers blood sugar balance and mind-body harmony with targeted supplements like berberine, chromium picolinate, Ceylon cinnamon, and GLP-1 support formulas that enhance insulin sensitivity, curb cravings, stabilize glucose spikes, and promote steady energy/mood without crashes. From high-potency blood sugar specifics blends with turmeric and ACV to microbiome probiotics that optimize metabolic health via gut-glucose regulation, Kiwla’s range complements low-GI eating, post-meal walks, and stress management—delivering appetite control, fat-burning support, and neurotransmitter stability for clearer focus, resilience, and sustainable weight goals. Easily accessible online in India, these science-backed essentials make daily habits like protein-first meals and vinegar hacks even more effective for metabolic vitality.
Conclusion:
Understanding the intricate relationship between blood sugar, mood, and metabolism empowers individuals to take proactive steps toward holistic well-being. By recognizing the mind-body connection, you gain the ability to make evidence-based decisions that support emotional balance and metabolic efficiency. Embracing this knowledge fosters resilience and promotes sustained wellness, underscoring the importance of personalized strategies in managing your health. Ultimately, cultivating awareness and control over your blood sugar is a vital component in achieving long-term vitality and a balanced mood.
Recent Posts
-
Modern Beauty Minimalism: How Ghost Lashes and Bare-Glam Are Changing Beauty Standards
Introduction: Beauty trends have always been cyclical, but the latest sensation sweeping through Ind
-
The Fungus Inside Us: How the Mycobiome is Linked to Cancer
When we think about the organisms within us, the first thought is often bacteria—the gut microbiome
-
Scalp Therapy Isn’t Just a Trend—It’s the Next Big Haircare Routine
Introduction:Scalp therapy isn't just a trend—it's the next big haircare routine that's changing how